Venous ulcers are chronic wounds that struggle to heal naturally without intervention. These open sores typically appear on the lower leg or ankle, and they result from underlying issues with blood circulation. Proper diagnosis and medical treatment help resolve the wound, improving the patient’s quality of life.
What Are Venous Ulcers?
Venous ulcers are open wounds that develop when the veins in the legs fail to circulate blood back to the heart efficiently. This condition leads to high pressure in the veins, which eventually damages the skin until it breaks. They are distinct from arterial ulcers, and they require a specific treatment approach focused on restoring venous health.
What Causes Them?
The primary cause of these ulcers is chronic venous insufficiency. This condition occurs when the one-way valves in the veins malfunction. When these valves become damaged, blood flows backward and pools in the lower extremities, causing swelling and tissue damage. The constant fluid buildup deprives the skin of oxygen and nutrients over time, and the tissue begins to break down.
Several factors increase the risk of developing venous insufficiency, including age, obesity, and a family history of vein disease. A history of blood clots can damage the valves, and a sedentary lifestyle may weaken the calf muscles that pump blood. Addressing these risk factors is part of a comprehensive treatment plan.
What Are the Symptoms?
Patients may notice changes in the skin before the ulcer forms. These changes include discoloration or tissue hardening. The area may become itchy or swollen, with the skin looking shiny, tight, or reddish-brown. Once the skin breaks, the ulcer appears as a shallow wound with irregular borders, and it may be accompanied by leg pain or heaviness.
What Treatments Work?
Effective management begins with specialized wound care to create an environment conducive to healing. Healthcare providers clean the wound to remove dead tissue, and they apply specialized dressings to control moisture levels. Compression bandages are then applied to the leg, which helps the veins pump blood more effectively.
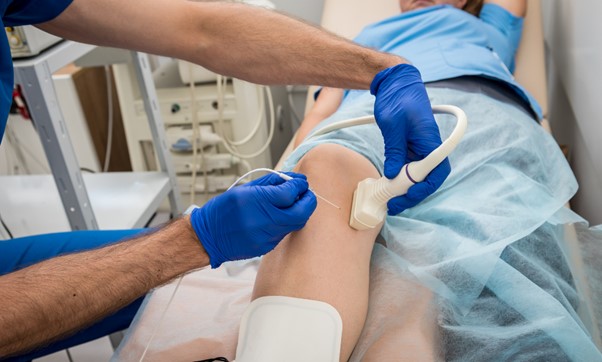
Ultrasound-guided sclerotherapy addresses the underlying venous insufficiency by chemically sealing the diseased veins. A physician uses ultrasound to visualize the vein, and they inject a sclerosant solution directly into the vessel. The solution irritates the vein lining, causing it to collapse and eventually be absorbed by the body.
Endovenous laser therapy (EVLT) is a minimally invasive option that uses thermal energy to treat the incompetent vein. A thin fiber is inserted into the vein, and laser energy is delivered to seal the vessel shut. This procedure diverts blood flow to healthy veins, reducing venous pressure that causes the ulcer. Varithena® foam sclerotherapy is another treatment option for varicose veins and venous reflux.
What Are the Benefits?
Treating the underlying cause of venous ulcers promotes faster healing and helps lower the risk of recurrence. Patients may report reduced pain and swelling, and they may see an improvement in the appearance of their legs. These minimally invasive treatments allow for a quick return to daily activities, with minimal disruption to the patient’s life.
Seek Treatment Today
Venous ulcers are a complex medical condition, but effective treatments are available to restore vein health. Early intervention prevents complications and helps patients regain mobility and comfort. Schedule a consultation with a vein specialist today to determine the most appropriate treatment for your vascular health.